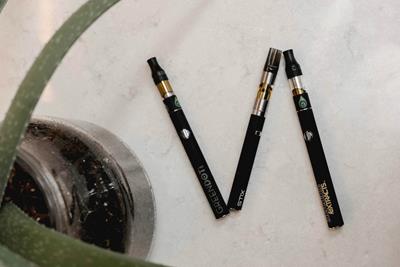Are Some Vape Cartridges Contaminated by Heavy Metals and Lead?
- Thursday May 25, 2023
States are effectively forced to allow for small amounts of lead because it is so cost-effective for the companies that use it. Lead is often tempered into other metals to make them cheaper and more flexible.